Cree Lighting® CONNECTED MAX® Smart LED Bulb with Variable Color Temperatures and Color Changing Options | CMPAR38-120W Series | 14W | 2200K-6500K | White

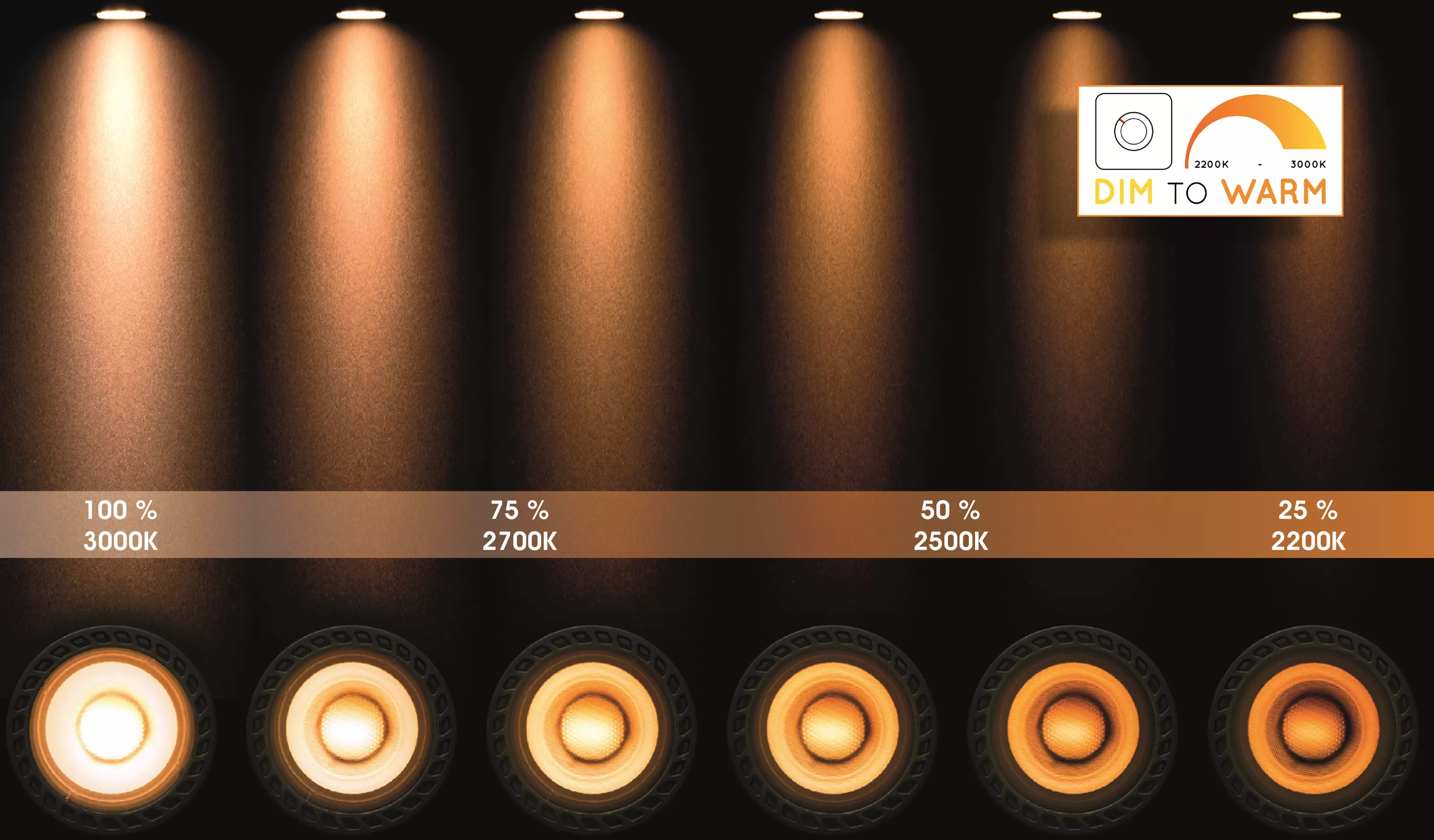
Lucide TAYLOR - Ceiling spotlight Bathroom - LED Dim to warm - GU10 - 1x5W 2200K/3000K - IP44 - Black | ideas4lighting

LEISO New Design SCOB GU10 LED Bulbs 6W 80 To90RA Dimmable And Non-Dimmable 2200K To 5500K Color Temperature - LEISO 3D

Philips Lighting 4GU10/LED/927-22/F35/G/WG/T20 10/1 :: 4.5W LED PAR16 GU10 Bulb :: PLATT ELECTRIC SUPPLY